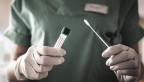
The Cornell COVID-19 Testing Laboratory, housed in the College of Veterinary Medicine, is a cornerstone of the university’s efforts to conduct continual testing of the campus population.
Teaming up: Coronavirus research at Cornell
By J. Edward Anthony
Bacteria that churn out a COVID-19 vaccine like tiny pharmaceutical factories.
An antibody test that not only indicates whether you’ve been exposed but also measures the strength and progress of your immune response.
A friendly giant of a molecule, harmless to humans that, once injected into the bloodstream, will bind like Velcro to the outside of SARS-CoV-2, keeping it from doing harm by holding the virus in a relentless molecular bear hug.
To people anxious for practical help, these ideas might sound far-fetched – but to Cornell researchers working at the forefront of their fields, these outside-the-box, collaborative approaches are full of possibility. All are based on concepts and technology that were previously developed at Cornell to address other engineering, diagnostic and clinical challenges. Now Cornell researchers are re-examining and adapting their innovations to develop the tests, treatments and knowledge necessary to end the COVID-19 pandemic.
Earlier this year, the three projects mentioned above, along with 20 others, received Phase I funding through the OVPR SARS-CoV-2 Seed Grant program, a joint endeavor of the Office of the Vice Provost for Research (OVPR), the Center for Vertebrate Genomics and the Center for Immunology. OVPR Seed Grants are giving researchers the extra financial support they need to pivot their expertise and technical resources toward this global health crisis.
“Through the OVPR Seed Grants, we were able to fund a lot of genuinely innovative, interdisciplinary collaborations – projects involving researchers from multiple colleges, multiple departments and people who you would not consider to be traditional virologists,” says Paula Cohen, professor of genetics and associate vice provost for life sciences. “This cooperativity is what Cornell does best.”
Generating preliminary data
“There is a sense of obligation to help fight the pandemic, and there’s lots of urgent funding for COVID-19-related research out there,” says Ailong Ke, professor of molecular biology and genetics. “But for people like me, with relevant expertise and ideas but no direct experience with virology, [the OVPR Seed Grant] is the resource I needed to move forward and generate data that will convince external funding sources to fund my idea directly.”
Ke – in collaboration with Hector Aguilar-Carreno, associate professor of microbiology and immunology in the College of Veterinary Medicine, and Robert Dick, a research associate in the Volker Vogt Lab in Molecular Biology and Genetics – is engineering a molecular decoy that the SARS-CoV-2 virus will find more attractive, from a biochemical standpoint, than the receptors on human cells that the virus typically exploits.
“To work, these receptor-like decoys will have to have an advantage,” Ke says. “They’ll have to have greater affinity and bind more tightly to the virus than a cell’s surface receptors do. Basically, they will latch onto the viruses and then sequester them away.”
The strategy has some similarities to a successful antibody treatment for the Ebola virus, but Ke hopes that decoy receptors will have some advantages over antibody treatments.
“The [SARS-CoV-2] virus may mutate and weaken the effectiveness of a particular antibody. But the virus will always target the same receptors on cells,” Ke says.
Overcoming unforeseen obstacles
“When we all found ourselves in this situation – to do COVID-19 research or not – anybody with a good idea was very clearly motivated to do something,” says Bettina Wagner, professor of population medicine and diagnostic sciences. Wagner and collaborators at the College of Veterinary Medicine and the Animal Health Diagnostic Center (AHDC) are developing an antibody test based on the same technology that the AHDC uses for its Lyme disease test.
The AHDC already has the capacity to run hundreds of multiplex antibody tests per day for Lyme disease, and Wagner believes they can do the same for COVID-19. Because multiplex tests at the AHDC simultaneously detect multiple proteins associated with a particular pathogen, they are more sensitive and accurate than tests based on a single antigen. With the additional data, researchers can also detect patterns in people’s varied immune responses, which could eventually allow researchers to estimate when exposure to the virus took place and the strength of a person’s immunity.
The incentive was already there – “I was absolutely committed to doing the work,” Wagner says – but an OVPR Seed Grant helped her overcome the unforeseen obstacles that can arise when advancing an urgent research agenda. Wagner and her collaborators needed blood serum from a large number of healthy individuals, including some who had been exposed to the virus and already recovered, to develop the multiplex test.
She turned to the Cornell community.
“Very rapidly, we organized this healthy volunteer clinic here at the College of Veterinary Medicine to collect serum,” Wagner says, “and I was able to use the [OVPR] Seed Grant to cover some unexpected costs. It really helped me quickly gather the data we needed to progress.”
Promising innovations
David A. Putnam, professor of biomedical engineering, and Matthew P. DeLisa, the William L. Lewis Professor of chemical and biomolecular engineering, recently garnered $17.9 million from the National Institutes of Health to develop their idea for an ingenious new vaccine technology.
Working with Gary Whittaker, professor of virology in the College of Veterinary Medicine and a section chief in infectious disease epidemiology in the Master of Public Health program, Putnam and DeLisa are gunning for a universal, once-and-for-all, seasonal flu vaccine. As their flu vaccine progresses toward human trials, they are working to adapt the new platform for COVID-19.
The new vaccine platform delivers immune-triggering antigens in packaging made from the outer membrane of bacteria. In fact, specially engineered bacteria actually manufacture the vaccine from their own cells. Certain bacteria have the peculiar habit of developing tiny blisters on their outer membranes that bud and break away, forming what are called outer membrane vesicles [OMVs]. These OMVs are not themselves bacteria, but they contain some fluid and other contents of the bacteria that made them – including, in this case, proteins from the SARS-CoV-2 virus that the bacteria will be engineered to mass produce.
The resulting OMVs are harmless, but their bacterial membrane puts the human immune system on alert – provoking a strong response to the antigens contained within. “To the immune system, it looks like the virus,” Putnam says. “But functionally it's nothing like the virus. It just has proteins from the virus.”
Putnam speaks of the OVPR Seed Grant with the energetic, rapid-fire enthusiasm of a varsity coach.
“I work with this fantastic graduate student, Mariela Rivera de Jesus, who is engineering the immune response for the flu vaccine,” says Putnam. “And I said, ‘Hey, Mariela, do you want to try this on COVID?’ Mariela says, ‘Yeah, sure, let's go!’ But we didn't have the money. We had the technology. We had talented students with the expertise we needed, like Mariela and Stephanie Curley, a postdoc on the project. But we didn’t have the money to go for it. Then we won [the OVPR Seed Grant] to find the reagents, so now we’ve started working on the vaccine itself.”
The OVPR SARS-CoV-2 Seed Grant program awarded more than $200,000 to 23 projects this summer during initial Phase I funding. During Phase II this fall, awarded projects will be considered for additional funding that will total another $200,000 across the program. Decisions will be based on the project’s scope and the strength of its Phase I results, with Phase II distributing larger awards to a smaller number of projects.
“The OVPR’s mission, along with that of our funding partners in this endeavor, is at the heart of this program,” Cohen says. “With the seed grants, we did exactly what we set out to do – namely, to bring fantastic scientists to the table from all corners of the campus to address this global pandemic.”
A version of this story originally appeared on the Cornell Research site.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe