Multiplexed C dots track cancer cells to improve patient care
By David Nutt
For more than a decade, researchers have used glowing nanoparticles called Cornell dots, or C dots, to illuminate cancer cells, target tumors and even induce cell death.
Now, a new iteration of C dots is expanding their impact through fluorescence-based multiplexing, a process in which multiple C dots are dispatched to track different cancer targets.
C dots, which are made of silica, are able to track cancer cells because they are equipped with targeting molecules that home in on the presence of overabundant proteins on a tumor cell’s surface. The search can be complicated by the fact that tumor cells are heterogeneous, with numerous compounds being overexpressed at different times as the disease progresses. Tracking only one of these markers is therefore risky.
Deploying several multitasking C dots allows researchers to navigate these shifting variables and detect multiple cancer markers simultaneously during surgery in a way that is both precise and safe. The process could help surgeons and oncologists make more informed decisions about which therapeutic regimen should follow surgery.
“We basically took the first application of the C dots, which was nodal mapping, and moved to the next stage,” said Ulrich Wiesner, the Spencer T. Olin Professor of Engineering in materials science and engineering. “Rather than mapping based on a single fluorescent marker that is specific for a single receptor overexpressed on the particular tumor cells, here we can multiplex and look at multiple markers simultaneously in order to assess the heterogeneity of the tumor.”
The resulting paper, “Molecular Phenotyping and Image-Guided Surgical Treatment of Melanoma Using Spectrally Distinct Ultrasmall Core-Shell Silica Nanoparticles,” published Dec. 4 in Science Advances.
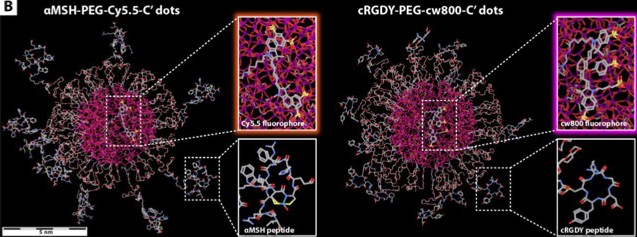
Wiesner’s group worked with longtime collaborator Dr. Michelle Bradbury and her team at Memorial Sloan Kettering Cancer Center (MSKCC). They focused their C dots on two different markers known to be overexpressed in human melanoma: integrin alpha-V and melanocortin 1 receptor (MC1-R). While MC1-R is largely specific to melanoma, alpha-v beta-3 is also expressed by a variety of other solid tumors.
As in previous studies, the team targeted the lymphatic system because when tumors metastasize, the cancerous cells shed material that nests in the lymph nodes, forming secondary lesions that can spread throughout the body.
Before starting the surgery, the researchers labeled their C dots with a radiotracer and injected them near the primary melanoma of the patient – in this case, a miniature swine. The researchers used a combination of imaging techniques – positron emission tomography and X-ray-based computed tomography – to track the particle tracer as it moved through the tumor-draining lymphatics and located the diseased lymph nodes and other cancerous lesions. Once the lymph nodes were localized, the miniswine was taken to the operative suite and injected, near the lesion, with a cocktail of two different C dots, each distinguished by different fluorescent colors.
The dots also were coded with two different targeting systems: cyclic RGD, which seeks out the integrin alpha V, and alpha-MSH, which seeks out MC1-R. With the aid of a multi-channel fluorescence camera system that was adapted specifically for multiplexing, the surgeons followed the glowing C dots to their respective target receptors on the surface of the cancer cells where the different colors simultaneously revealed heterogeneities in the expression levels of the two markers.
After the lymph nodes were removed, the researchers used pathology tests to confirm the presence of the markers, as well as determine the amount of cancer within the nodes. The findings showed a strong correlation between tumor size and florescence intensity: the stronger the signal, the larger the tumor. The multiplexing C dots also enabled the researchers to detect elusive micrometastases – very small tumors, less than 2-3 millimeters in diameter. The team found micrometastases as small as 0.45 mm in some lymph nodes.
“This is important because there’s a lot of questioning about whether the particles are sensitive to the tumor or if they’re sensitive to some other cells that are present in the lymph nodes as a result of the tumor,” Wiesner said. “Demonstrating that there’s a correlation between tumor burden and the amount of fluorescence intensity we measure shows that the C dots are specific to the tumor.”
The researchers conducted their trial in miniature swine to reproduce the human-patient environment as much as possible, preparing the way for clinical trials.
“This is an achievement in the sense that what has been promised for decades in using multiplexed optics in the surgery room has now been demonstrated as close to the real thing as you can possibly go,” Wiesner said. “We show that these multiplexed approaches work, and work really well.”
“Our ability to use these cancer-targeted C dots as imaging ‘biomarkers’ to detect micrometastases in lymph nodes may allow us to non-invasively stratify patients to different treatment arms and make more efficient surgical management decisions,” said Bradbury, who is the paper’s co-senior author and director of intraoperative imaging and professor of radiology at Sloan Kettering Institute for Cancer Research and Weill Cornell Medicine.
Co-lead authors were postdoctoral researcher Kai Ma in the Department of Materials Science and Engineering, and Feng Chen and Brian Madajewski with MSKCC. Snehal Patel of MSKCC was co-senior author. Ph.D. student Melik Z. Turker and researchers from MSKCC, University of Missouri and Quest Medical Imaging also contributed to the paper.
The study was supported by the National Institutes of Health and Sloan Kettering Institute.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe