Ankur Singh, left, works in his lab with doctoral student Sungwoong Kim.
Immune-engineered device targets chemo-resistant lymphoma
By Tom Fleischman
Non-Hodgkin lymphoma, a cancer that is diagnosed in the U.S. more than 70,000 times annually, arises from overly proliferating immune cells within the body’s lymph nodes, which are connected to a network of lymph vessels through which lymphatic fluid flows.
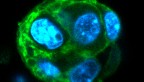
The most common type of lymphoma is diffuse large B-cell lymphoma (DLBCL), accounting for about 1 in 3 lymphomas, and approximately half of these tumors are resistant to chemo-immunotherapy. Once the lymphoma originates in a lymphoid tissue, cell proliferation causes rupture of the tissue’s overall structure, and the cells are exposed to mechanical forces such as fluid flow.
The lab of Ankur Singh, assistant professor in the Sibley School of Mechanical and Aerospace Engineering (MAE) and the Meinig School of Biomedical Engineering (BME), has partnered with researchers at Weill Cornell Medicine to explore how these fluid forces may relate to the tumors’ drug resistance.
The Cornell team – which includes Dr. Ari Melnick, the Gebroe Family Professor of Hematology/Oncology and professor of medicine at Weill Cornell Medicine – has developed a “lymphoma micro-reactor” device that exposes human lymphomas to fluid flow similar to that in the lymphatics and parts of the lymph node.
Their paper, “How Biophysical Forces Regulate Human B Cell Lymphomas,” was published April 10 in Cell Reports. Lead author is FNU Apoorva, Ph.D. ’17; also contributing was assistant professor Benjamin Cosgrove (BME) and professor Brian Kirby (MAE).
“This project used highly interdisciplinary approaches, from mechanical to biomedical engineering,” Apoorva said, “and interfaced with the clinical side of lymphomas [with Melnick] to help explain the role of fluid forces and nutrient transport on resistant tumors.”
The group’s side-flow micro-reactor includes a cell culture chamber connected to a media (fluid) chamber by narrow resistance channels, which slowed the fluid to mimic the flow inside lymph vessels and parts of lymph node.
In testing different subsets of DLCBL lymphoma, the group discovered that certain subsets, classified based on mutations in B cell receptor molecules found on cell surfaces, responded differently to fluid forces. Most notably, the team discovered that fluid forces regulate expression levels of adhesion proteins known as integrins, as well as B-cell receptors.
The team found cross-talk between integrin and B-cell receptors signals that could help explain certain tumors’ drug-resistance.
“It is pretty remarkable that subclasses of the same tumor respond differently to mechanical forces,” said Singh, the paper’s senior author. “If we can understand the role of all these biophysical stimuli, we may understand why some lymphomas are sensitive to treatment while others are refractory. Then we will be able to treat many more patients.”
This is the team’s first step toward modeling lymphatic systems and the effects of fluid flow on them, which they plan to further modify with relevant lymphatic cells and use for understanding immunity and malignancy.
“Understanding factors that regulate B-cell receptor signaling is important because this pathway is a key target for new classes of therapeutics,” said Singh, a member of the Caryl and Israel Englander Institute for Precision Medicine at Weill Cornell Medicine. “Several of these are in clinical trial stages.”
Melnick, who has collaborated with Singh on research related to organoids for the study of the immune system, said this work is important for several reasons.
“It shows that the underlying biology of lymphoma cells is linked to the physical properties of the host microenvironment,” said Melnick, who is a member of the Sandra and Edward Meyer Cancer Center at Weill Cornell Medicine. “Also, we show that certain physical properties of the microenvironment determine the activity of some of the key oncogenic gene pathways that drive the biology of lymphoma cells. This is missed in the typical studies where cells are simply grown in liquid culture.
“Ours is a novel approach for growing lymphomas in a more physiologically relevant context,” Melnick said.
Other contributors included doctoral students Alexander Loiben (BME) and Shivem Shah (BME); Alberto Purwada, Ph.D. ’17, formerly of the Singh Research Group; Lorena Fontan, an instructor of pharmacology in medicine at Weill Cornell Medicine; and Rebecca Goldstein, a former postdoc from the Melnick Lab.
This work was supported by grants from the National Institutes of Health and the National Science Foundation, as well as a Department of Defense Career Development Award to Singh. Some of the work was performed at the Cornell NanoScale Science and Technology Facility, which is supported by the NSF.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe