Study identifies human microRNAs linked to Type 2 diabetes
By Krishna Ramanujan, Cornell Chronicle
MicroRNA (miRNA) molecules in pancreatic islets have been thought to play important roles in Type 2 diabetes, but until now scientists have not confidently identified which miRNAs are associated with the disease in humans.
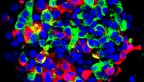
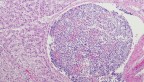
A new study, published Feb. 9 in the journal Proceedings of the National Academy of Sciences, represents the largest study to date of diabetes-linked miRNAs found in human pancreatic islets – groups of cells in the pancreas that secrete insulin and regulate blood glucose levels.
Most prior attempts to comprehensively profile miRNAs (which regulate which genes are turned on and off) in pancreatic islets using next-generation sequencing technology have been done in culture or with rodent models. A few studies conducted with hard-to-acquire human islets were limited by a small number of samples.
The study’s corresponding authors, Praveen Sethupathy ’03, professor of biomedical sciences in the College of Veterinary Medicine and director of the Center for Vertebrate Genomics at Cornell University, and Dr. Francis Collins, former director of the National Institutes of Health (2009-21) and a senior investigator at the National Human Genome Research Institute at the NIH, had access to a network that supplied nearly 65 human pancreatic islet samples from cadavers for this study.
The robust sample size allowed the researchers to use large-scale, next generation sequencing to identify at least 14 pancreatic islet miRNAs that are implicated in human Type 2 diabetes.
“We’ve defined in the largest cohort of human islets to date the miRNAs that might be most relevant for Type 2 diabetes,” said Sethupathy, who was a postdoctoral researcher in Collins’ NIH lab from 2008-11.
“We [also] found that some of the diabetes-associated miRNAs in humans are not ones that have been well-characterized in the previous two decades of studying islets and diabetes in rodent models,” he said.
MiRNAs were first found in animal cells in 2001. Soon after, in 2004, one of the first studies demonstrating their importance to physiology focused on a miRNA that regulates the function of pancreatic islets. Since then, hundreds of studies on miRNAs with potential relevance to pancreatic islets have been published, but few have used human tissue samples and none have been at the scale of this study.
“There’s been long-standing interest to better understand the molecular environment of the pancreas, so that we could get a better handle on what goes awry in diabetes patients and then eventually be able to use that information to develop better therapeutics,” Sethupathy said.
The relatively large sample size helps to reveal the extent of variation in the quantity of miRNAs in the islets, or expression level, across the human population. The researchers also had genetic information on all the patients, which helped them determine a handful of genomic loci underlying variability in miRNA expression, though ultimately this type of inquiry will require many hundreds of samples for a fuller picture. One of these loci was found in the same area of the genome that is associated with Type 2 diabetes-related traits, which could suggest a novel mechanism for how Type 2 diabetes develops.
Some of the most altered miRNAs in islets from individuals with Type 2 diabetes were consistent with those found in previous rodent studies, but there were also some notable differences. “These represent interesting candidates to investigate further in human models of pancreatic islets,” Sethupathy said.
In the future, researchers will need to further invest in the development and study of human models of Type 2 diabetes, such as genetically-modified islets or organoids, Sethupathy said.
Henry Taylor, an NIH trainee in Collins’ lab, is the paper’s first author. Other key coauthors include D. Leland Taylor, a postdoctoral fellow in Collins’ lab, and Yu-Han (Amy) Hung, a former postdoctoral fellow in the Sethupathy lab.
The study was funded by the National Institutes of Health, the Gates Cambridge Trust and the American Diabetes Association Pathway to Stop Diabetes Program.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe