Chow hounds: Dog food trials soothe gastrointestinal illness
By Olivia M. Hall
Buddy, a fun-loving briard rescue dog, had always been full of energy. Two years ago, that suddenly changed.
“Out of the blue he started having serious issues when going to the bathroom and would sleep all the time,” says Buddy’s owner, Chris Hein of Saratoga Springs, New York. “We could not figure out what was wrong with him.”
Pamela Reppert ’78, D.V.M. ’86, the family’s veterinarian at the Saratoga Springs Veterinary Hospital, referred to the Cornell University Hospital for Animals.
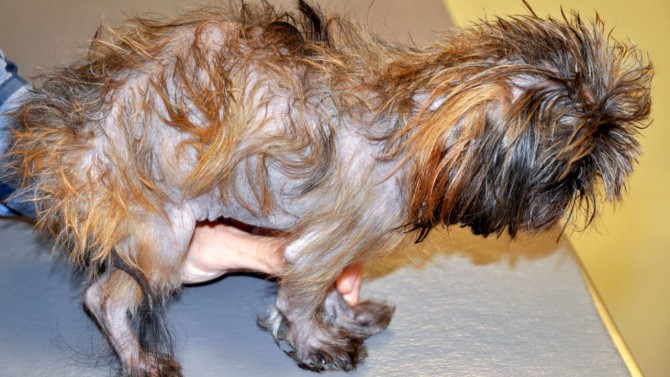
There, he became one of three dozen dogs thus far to participate in an ongoing study on treating persistent gastrointestinal problems, or chronic enteropathy, with changes in their diets. The results so far have been remarkable, with patients like Buddy, now 13, returning to healthy weights; others have regained glossy coats after being nearly hairless.
Most dogs with these kinds of persistent gastrointestinal problems have a form of inflammatory bowel disease called lymphocytic plasmacytic enteritis. Up to 80% of dogs with the disease respond well to changes in the food they eat, says Kenneth Simpson, professor in the College of Veterinary Medicine’s Department of Clinical Sciences and lead investigator for the study.
Veterinarians commonly prescribe foods that are more easily digestible or lack problematic ingredients, particularly meat-associated proteins that are thought to provoke an inflammatory response. More recently, pet food companies have created hydrolyzed diets in which the proteins are chemically “smashed” into smaller pieces to potentially avoid stimulating the animals’ immune systems.
“But no one really knows why or how these diets work or why the original diet caused clinical signs,” Simpson says. “We don’t know the optimal way to manage those dogs.” As a result, patients may undergo a whole slew of best-guess treatments as owners and veterinarians try to give them relief.
The Cornell study, Simpson hopes, will bring scientific rigor and more clarity to the process.
Since the study began in early 2018, the canine participants – recruited from the animal hospital and referring veterinarians – are separated into three groups: two receiving hydrolyzed protein diets, and one control group eating a high-quality maintenance mixed-protein diet. All the food contains the same balance of carbohydrates, protein and fat and is provided at no cost to the owners by the study’s sponsor, the pet food company Farmina.
A separate group consists of more severe cases such as Buddy, who suffer from a disease known as protein-losing enteropathy. The prognosis for these dogs is grim: About half die from the disease. Evaluating the effect of diet in these dogs is problematic, as many do not want to eat the prescribed food. For Cornell’s clinical trial, these dogs receive either of the two hydrolyzed diets, with the primary goal of increasing their interest in eating the new diet and gaining weight.
“If an animal in any of the groups fails to respond after two weeks, it can be crossed over to receive another diet, so it receives sequential therapy,” says Simpson.
The results so far have been positive, even dramatic, for many of the dogs. Buddy, too, has noticeably improved. His stools are nearly consistently solid, he rarely has gas and has regained 25 pounds. “He has been much more comfortable and less restless,” says Hein, who no longer gets up every night to let his dog out. “He’s almost completely back to his normal self.”
Simpson, while pleased, is a bit surprised at the preliminary results, which have not yet undergone final analysis. “Conventional wisdom would suggest that [dogs on] the hydrolyzed diets would do better and dogs on the intact mixed-protein maintenance diets would fail to respond,” he explains. Yet at three months, almost all dogs, regardless of their diet, have had positive responses. That means the placebo group is performing equally well.
Why changing diets has such a dramatic effect on dogs with chronic gastrointestinal disease remains unclear. Simpson hypothesizes that “the positive responses … are not a simple allergic response to intact protein. Perhaps nonprotein ingredients or additives may be causing adverse reactions.”
Simpson hopes that in-depth analyses of the participants’ gut bacteria and metabolism will provide additional insights to improve diagnosis and therapy. “Chronic diet-responsive enteropathy is one of the most common diseases we see,” he says. “Once we’ve analyzed the evidence thoroughly, I hope we’ll be able to make rational recommendations. That’s very heartening.”
This article is adapted from the original, “CVM clinical trial yields positive yet puzzling outcomes,” by Olivia M. Hall, a freelance writer for the College of Veterinary Medicine.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe