Knitted robotic textile promising for hand edema patients
Knitted robotic textile promising for hand edema patients
By Tom Fleischman, Cornell Chronicle
The best current treatment for hand edema – swelling caused by excess fluid accumulation, from injury or disease – is manual edema massage (MEM) by a trained therapist, but access to care and cost can make the procedure prohibitive.
Cindy (Hsin-Liu) Kao, assistant professor of human centered design in the College of Human Ecology and director of the Hybrid Body Lab, and her team have developed a solution that has the potential to be personalized and used in the comfort of one’s own home.
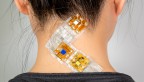
Working with physicians at Weill Cornell Medicine and therapists at the Cayuga Medical Center (CMC) Department of Physical Therapy, Kao’s lab has devised a knitted wearable technology, called KnitDema, that can gently massage the swollen area through sequential compression by small robotic actuators.
Heather (Jin Hee) Kim, a doctoral student in human centered design and Hybrid Body Lab member, is lead author of “KnitDema: Robotic Textile as Personalized Edema Mobilization Device,” which she will present April 26 at the ACM CHI ’23 Conference on Human Factors in Computing Systems, in Hamburg, Germany.
In addition to Kao, co-authors are Dr. Michael O’Dell, professor emeritus of clinical rehabilitation medicine at Weill Cornell Medicine; and Dr. Joan Stilling, assistant professor of clinical rehabilitation medicine at Weill Cornell Medicine.
The idea for KnitDema came following work on another wearable device, KnitDermis, which Kao’s lab developed more than three years ago. KnitDermis gives the wearer tactile feedback; it can pinch, twist and exert pressure on the wearer’s skin for a variety of purposes.
“In the user studies for KnitDermis,” Kao said, “a lot of the feedback that we got from participants was that people were really interested in having something like a personalized on-skin massage device, or for acupressure to serve their individual needs.”
That got Kao and her lab talking with O’Dell and Stilling at Weill Cornell Medicine, and they spent many weeks discussing the optimal target for this type of wearable. They chose hand edema, particularly swelling of the fingers, “because it’s a condition that affects a lot of people and can have significant impact to activities of daily living, since finger mobility is indispensable in our day-to-day lives,” Kao said.
Stilling appreciated being able to offer input during the device’s development.
“Usually, clinicians are presented with a technology to be implemented into the health care setting without having any input into design,” she said. “There are important considerations for use of the device in the medical context, and we were able to communicate and help to clarify important design features to the engineering team.”
Kim and Kao devised a knitted robotic textile to be put over a single finger, with thread-like shape memory alloy (SMA) springs woven into the knitted material. The springs are activated by a small printed circuit board, and compress sequentially to mobilize fluid out of the swollen area.
The duration and intensity of SMA spring compression is adjustable depending on the needs of the individual patient. The transition temperature at which the springs contract was 45 degrees Celsius (113 degrees Fahrenheit), which participants tolerated without discomfort, according to the paper.
Kao and Kim tested KnitDema on a simulated finger (a saturated sponge encapsulated in silicone). They designed the device to be comfortable to wear and quiet, with a more evenly dispersed compression around the swollen area as compared to MEM treatment.
In addition to the active compression, the device itself is made with a stretchy yarn – with hollow pockets for the actuators built in – that offers a tight fit and passive compression even when the actuators aren’t on. “We experimented with a lot of different types of yarn and novel knit structures,” Kao said, “to identify the unique combination that would be effectively compressing but not uncomfortable.”
Kao sees KnitDema, and potential other devices using this technology, as a “personalized rehabilitation device,” a term coined by the team as something that could be prescribed to an outpatient, as would a medication.
“Instead of having to schedule a hard-to-get visit with a therapist for MEM,” she said, “we envision this as something that people could take home with them. They would go to their rehab doctor and their occupational or physical therapist once, and at that session they would be able to configure the right amount of compression for daily use, then adjust as necessary.”
“It also allows for use any time that is convenient for the patient – often when symptoms are worst for the individual,” Stilling said. “In addition, each device is personalized for each person through the digital machine knitting, allowing for a customized fit, which is not readily available through standard treatment options on the market.”
Kao and Kim gave credit to physical therapists at CMC – particularly Allison Howe, whose certification includes lymphoedema – and the physical and occupational therapists at Weill Cornell Medicine for helping with the project. “They were really amazing collaborators,” Kim said.
This project was supported by a Cornell Multi-Investigator Seed Grant.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe