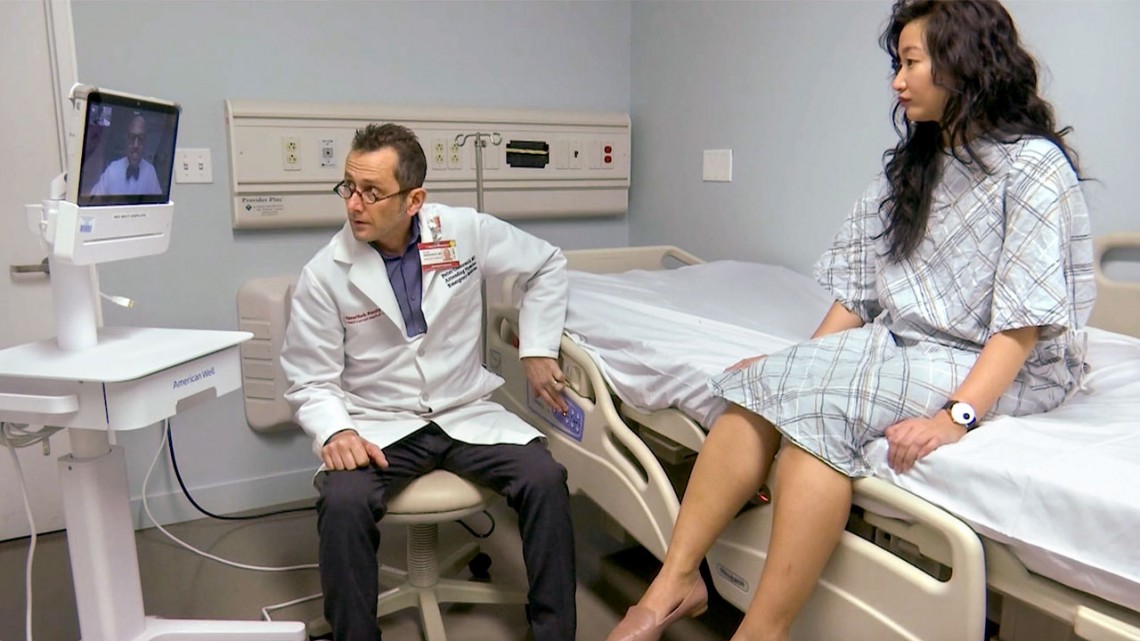
Dr. Peter Greenwald, center, and Dr. Neel Naik, on screen, demonstrate a telemedicine visit.
Telemedicine training proves vital during COVID-19 crisis
By Kathryn Inman
The doctor will see you now – virtually.
As hospitals and emergency departments urge more patients to stay home to avoid exposing themselves and others to COVID-19 and to reduce stress on the health care system, patient care has increasingly moved to web-based video and audio technology, called “telemedicine.”
The volume of virtual emergency medicine and ambulatory care visits, using NewYork-Presbyterian’s telemedicine service NYP OnDemand, has increased dramatically – from 20-40 patients per day in February to more than 300 per day in March, and the numbers continue to rise.
Similarly, primary care appointments using Weill Cornell Medicine’s Video Visits have gone up since the start of the COVID-19 crisis, with health care practitioners now fielding 700 virtual appointments per day.
Weill Cornell Medicine has been a leader in telemedicine training since it began working in the emerging discipline four years ago. Recognizing from the outset the importance of teaching virtual care skills and techniques to those practicing medicine, in addition to medical students, the Department of Emergency Medicine’s Center for Virtual Care (CVC) had successfully trained hundreds of its health care practitioners prior to the current health crisis.
Since then, the CVC has been at the forefront of this important initiative and trained more than 100 additional practitioners in a short period of time as it continues to broaden access to its program.
“This pandemic has highlighted the importance of broad, standardized telemedicine training of both our future and current providers,” said Dr. Rahul Sharma, professor and chairman of the Department of Emergency Medicine and executive director of the Center for Virtual Care at Weill Cornell Medicine, and emergency physician-in-chief at NewYork-Presbyterian/Weill Cornell Medical Center. “We want health care providers to be adequately prepared to give high-quality visits to our patients in this time of need and beyond.”
With health officials urging the practice of social distancing and discouraging in-person medical visits, both patients and providers nationwide have had to adapt. Recognizing a need to expand the reach of its telemedicine program, the CVC has created remote learning modules, moving its training online to get medical professionals trained as quickly as possible, ensuring that they are prepared to provide high quality care – as well as reassurance – for their patients.
“I believe we have put a lot of people’s minds at ease,” Sharma said. “Without this platform, people would be stuck in their homes and wouldn’t know who to talk to about their medical concerns. Now they can pick up their smartphone and reach a doctor. … This provides an opportunity to get that health care advice and peace of mind without making a trip to the ER.”
Launched in early 2020 to build on Weill Cornell Medicine’s existing telemedicine education program, which focused on medical students, the CVC now trains both students and health care practitioners in the fundamentals of virtual care. Through innovative teaching methods and classroom instruction, the training includes “web-side” manner, remote patient examination skills and how to make treatment-related decisions while using virtual media. Using simulations with standardized patients, trainees learn how to how to best present themselves on camera and to effectively interact with patients online.
“Telemedicine has ended up being the perfect tool to deploy during this health crisis, which requires us to limit physical contact,” said Dr. Neel Naik, the simulation education director for the Department of Emergency Medicine and an assistant professor of clinical emergency medicine at Weill Cornell Medicine.
“A stay-at-home order doesn’t mean that patient care stops,” said Naik, also an emergency medicine physician at NewYork-Presbyterian/Weill Cornell Medical Center. “There is still a lot of regular, ongoing medical care that needs to be provided, it just can’t be conducted in the traditional way of showing up to your doctor’s office.”
For a longer version of this story, visit the Weill Cornell Medicine website.
Kathryn Inman is associate editor for Weill Cornell Medicine.
Media Contact
Get Cornell news delivered right to your inbox.
Subscribe

